Pegasus Knowledge Center

The New Paradigm for RCM Companies - Why Scale Matters
Beginning in the early 2000's, pundits have forecast major changes for the healthcare industry, especially in the area of Revenue Cycle Management (RCM). With the passage of the Patient Protection and Affordable Care Act (PPACA) and the Health Information Technology for Economic and Clinical Health Act (HITECH) their prognostications were assured. Although the healthcare industry has been slow to adopt all of the technology that has been described in the forecasts, it is now clear that Electronic Health Records will be ubiquitous throughout all hospitals and medical practices by the end of 2015. Patient portals and the adoption of outsourced billing solutions are also being rapidly adopted as the technology matures and gains traction across the country. So clearly the future of RCM is already here. When we consider the automation that has been adopted in other industries we are left to wonder what else can the Healthcare Industry, and RCM process in particular do to reduce costs. By looking at what has already transpired in other industries we can predict some very important trends in the near future for the medical RCM process.
As the CEO of Pegasus Blue Star Fund, a private equity fund specializing in Healthcare Services Investments, I have over 20 years of experience investing and managing Healthcare Services companies in the areas of Cancer treatment centers, Surgery centers, Practice management, Medical Group Purchasing Organizations, EHR, Medical Revenue Cycle Management, Patient Portal, Claims Optimization, Claims Authorization, Patient collections, Bad debt collections etc. Based on my observations of the changes impacting the Healthcare Industry today I predict that the changes in the Medical RCM business in the next two years will be as tumultuous to the Healthcare Industry as the race to adopt ERP solutions to address the Y2K "issue" was to the Fortune 500 businesses in the waning years of the 20th century. The similarities are eye opening. In the late '90s businesses were scrambling to make major changes to their computer systems to accommodate the change in the century. Some companies made minimal changes and continued business as usual, while the creative and innovative companies used this issue to make major investments in their infrastructure and make major changes to processes and technology. The companies that did not use this external driver to optimize their processes and adopt new technologies found that they were having great trouble competing with the ones who had. They had fallen behind the technology curve and were no longer cost competitive The majority of the companies moving to new technology moved to integrated platforms such as SAP to deliver their new business solutions. Medical practices today are poised to adopt multiple disparate technical solutions to meet governmental dictates, payer mandates, and patient expectations. Currently the solutions that are available are fragmented and have limited ability to communicate with each other. The solution that is required for the healthcare industry must be holistic and fully integrated so that all processes can be optimized and automated while at the same time providing critical information on practice costs and operating performance to help maximize profitability by optimizing all business processes.
RCM companies today:
Today there are thousands of small RCM companies that are performing billing for medical practices, but their profits are dwindling due to the increased demands by payers for automation and increased governmental regulations which require constant retraining of staff and modifications to billing systems. ICD-10 alone will drive the number of codes available for billing from 17 thousand to over 140 thousand. This is both a staff training issue and a technology issue. Furthermore, the physicians expect and demand that the billing company provide the training they need to meet the new ICD-10 coding requirements. Small RCM companies are at a disadvantage here, because they do not have the funds or staff size to adequately respond to these new requirements.
ICD-10 is not the only change driver impacting RCM company performance. The EHR mandate and the move to hospital based practices are also having a negative impact on earnings and complexity, as the practices demand that the RCM companies automate the charge process and provide much more sophisticated reporting capabilities to meet the growing need for information to optimize their practices. Reports that provide excessive data and limited analytical capability are no longer acceptable and small RCM companies are unable to afford the required investment necessary to provide the automation, business intelligence reporting, and billing system upgrades.

The last nail in the coffin for small RCM providers is the advent of the new generation of medical practice service providers that offer a virtual smorgasbord of tightly integrated and automated services at rates that cannot be matched by the highly manual small RCM incumbents. Large RCM companies, like Constellation Healthcare Technologies, have the scale that allows them to leverage their size to provide state of the art technology and world class processes to ensure that their clients have the perfect suite of services to maximize their profitability.
The majority of industries today utilize Enterprise Resource Planning (ERP) systems to deliver the needs of sharing information with internal and external stakeholders in a quick and easy manner, while also providing real-time insight into the health of the business. The Healthcare Industry needs the same thing, but it needs to have insight into the health of the patient in addition to the health of the business.
Large outsource providers are all working on building the solution that will capture the imagination of the industry by seamlessly tying together all the key components of a hospital or medical practice. The future of the RCM business belongs to the largest RCM providers who can partner with the medical practice to deliver a holistic customized solution. These new partnerships will require major investments in technology, while maintaining the traditional highly personalized relationship with the practice managers and healthcare providers. Joe Seale, President of Orion HealthCorp, shared some of the components that he believes are needed to meet the needs of the Healthcare Practices of the future:
- Patient Scheduling, demographics, and pre-authorization,
- Symptom analysis and diagnostic support,
- Coordination and scheduling of test procedures and lab analysis,
- Treatment Planning and Prognostication support from Artificial Intelligence Tools and Databases,
- Use of Government and Private Knowledge Warehouses to assist with the diagnosis and treatment (e.g. Pharmacies, Centers for disease control, etc.)
- Electronic storage of patient record storage and retrieval,
- Voice recognition and automated transcription,
- Automated coding of procedures based on automated transcription,
- Automated quality control and coding audit,
- Automated claims with payers,
- Automated payments and denials,
- Complete integration of accounts receivable with treasury functions and accounting
- Complete integration of HR, Payroll, Benefits, Finance, Treasury, Accounting, Taxes, Financial Reporting and Controls, Purchasing and Logistics
- Electronic Data Interchange with suppliers and partners (Radiology, Labs, Payroll, Billing, etc.)
- Business Intelligence and Management Reporting
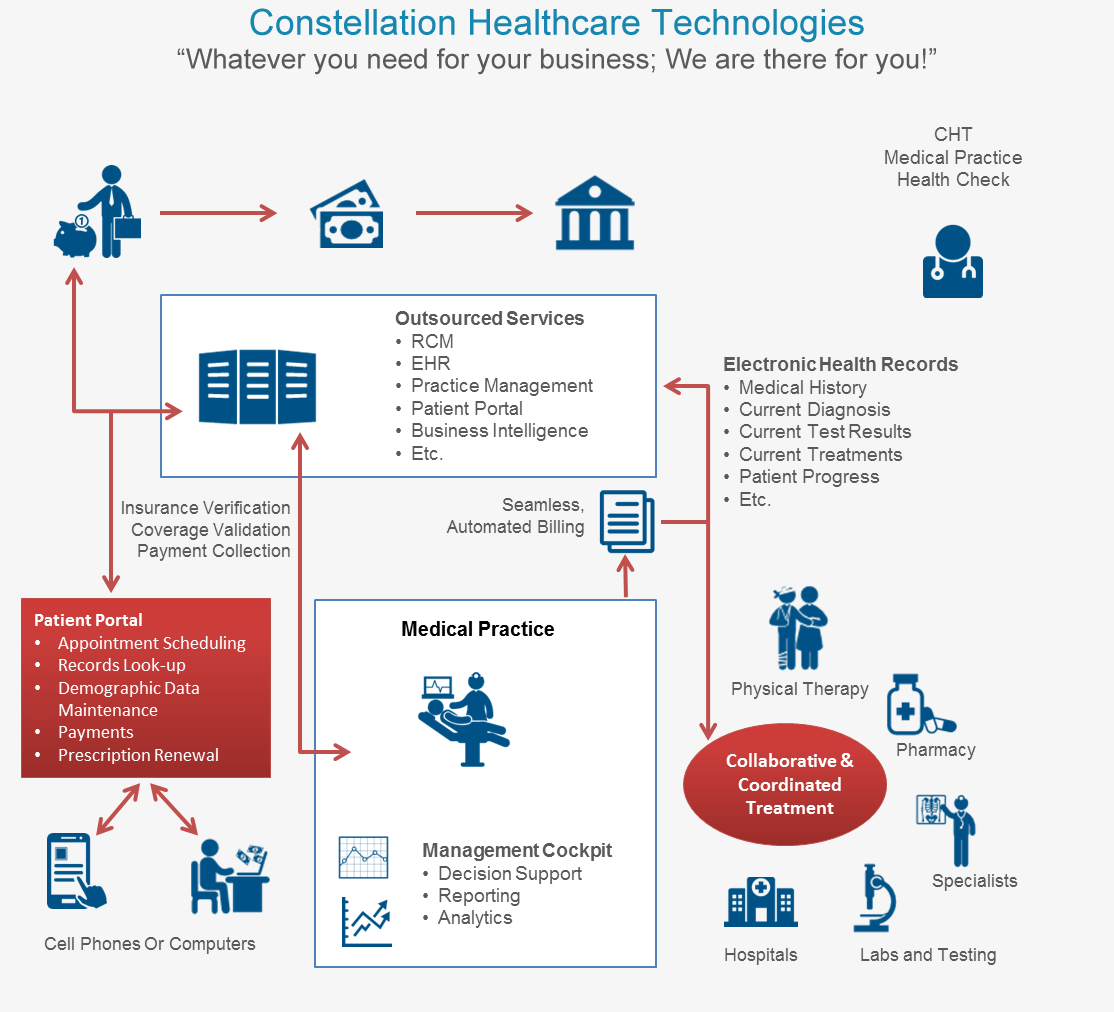
Full Service Medical Practice Service Companies of the future:
The figure below shows how the medical practice will rely on their service company for far more than billing, as the RCM industry morphs into a full service provider offering everything from billing to process improvement consulting, making these large innovative companies true partners with their clients and making the American dream of less costly high quality healthcare a reality.